We are open and safely seeing patients LEARN MORE
Love your legs.
Book now

Does insurance cover my vein treatment?
CLICK HERE TO FIND OUT FREE OF CHARGE
or
Simply call our complimentary medical insurance concierge now:
Our Vein Clinic is a Top-Rated Vein Center for Spider and Varicose Vein Treatment
Ivy League Doctors
Diplomate Certified
Ivy League Medical Directors
Did you know most vein treatments are covered by insurance? That’s not the only good news we’ll share at your initial consultation!
Get Hopeful. We Like to Change Lives.
We’ve helped over 10,000+ patients like you.
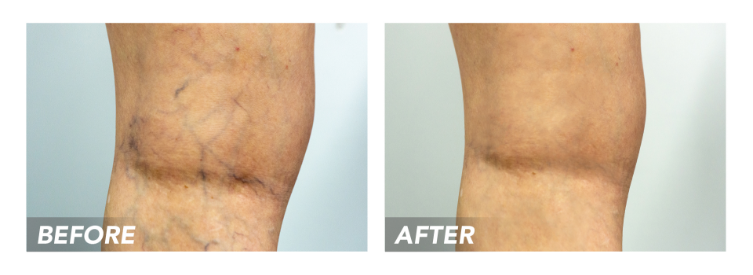
Check out their results:
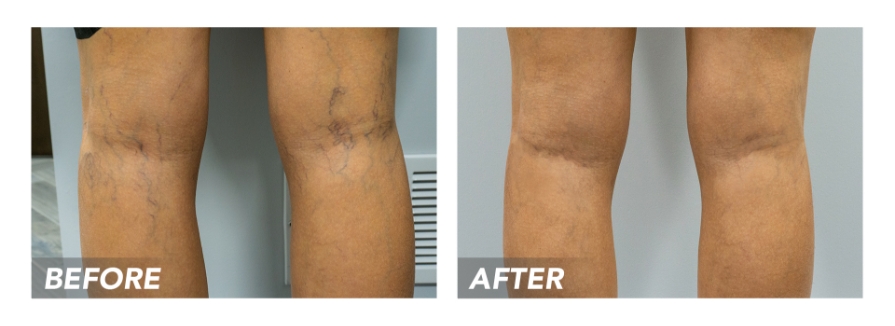
Before & After Gallery

Effectiveness

Likelihood of Insurance Coverage

Recovery Time

Customized Approach
![]()
![]()
![]()
![]()
![]()
Ready to Begin Your Vein Treatment Journey With Us?
Learn more about your vein condition and book a consultation today.
We look forward to meeting you. Got questions? Visit our Vein Treatment FAQ page.
Spider Vein Treatments
Varicose Vein Treatments
What Can I Expect from the Vein Treatment Clinic Closest to me?
Are you a new patient? Loved one, family member, friend or caregiver? Let us help you! Call us today at (888) 827-7441

Why Choose Our Spider and Varicose Vein Doctors?
OUR DOCTORS ARE CERTIFIED DIPLOMATES AND SELECTED BASED ON MERIT
You should always ask if your Vein Doctor is certified. Accreditation is important because that means that your vascular doctor has undergone the rigorous process of training and certification in their specialty.
Our medical directors trained at Harvard Medical School and oversee all quality control at our vein centers. We expect that our vascular doctors stay up to date on all technological advances in varicose vein treatment including Sclerotherapy and Radiofrequency Ablation.
WE WILL CREATE A CUSTOM TREATMENT PLAN FOR YOU IN THE SAFETY OF OUR HIGH-TECH CLINIC
Our medical directors are national experts in the venous field. Because of this, we are always up to date on the latest evidence-based approaches to treating vein disease. Our pre-op care, treatment options, and post-op care are based on the latest studies – this ensures that all of our patients get the best care – consistently. Lastly, because our doctors follow a standardized protocol, you can be assured that you will receive the same high level of care at all of our Vein Clinics.
WE TREAT THE ACTUAL UNDERLYING CONDITION TO PRESERVE LONGTERM HEALTH GOALS
Many vein clinics will offer only one procedure. At our vein centers in New Jersey, New York, Long Island, California and Maryland, we offer all the latest and safest vein treatment modalities in healthcare so we are able to customize a varicose vein treatment plan specific for your chronic venous insufficiency. With this unique approach, we are able to diagnose and treat your vein disease so that your legs not only look better, but also feel better. We look forward to caring for you and your loved ones!

Dr. Andrew Cortes
Vein Doctor New Jersey
SUNY Downstate Medical Center
Dr. Sahil Patel
Vein Doctor New Jersey
Rutgers University
Dr. Billy Schoenfeld
Vein Doctor San Diego
Harvard University
Dr. Juan Montoya
Vein Doctor New York
Yale University
Dr. Carly Guthrie
Vein Doctor San Diego
Harvard University
Dr. Shane Volney
Vein Doctor New York
Harvard University
Dr. Laura Lombardi
Vein Doctor New York
Harvard University
Dr. Kamran Saraf
Vein Doctor Maryland
University of Miami
Dr. Sareh Rajaee
Vein Doctor New York
Yale Medical School
Dr. Zalekha Shair
Vein Doctor Long Island
New York Medical College
Dr. Todd Kobrinski
Vein Doctor New Jersey
George Washington University
Dr. Walter Lech
Vein Doctor San Jose
Harvard University
Dr. Jeffrey Deygoo
Vein Doctor New Jersey
George Washington University
Dr. Thomas Arnold
Vein Doctor Long Island
University of Pennsylvania
Dr. Lisa Alford
Vein Doctor Maryland
McGill University
Dr. Jasmine Koo
Vein Doctor San Diego
University of Washington
Dr. Michael Nguyen
Vein Doctor
Harvard University
Dr. Caroline Novak
Vein Doctor
Northwestern University
Dr. Sahar Amery
Vein Doctor New Jersey
Stony Brook University Hospital
Dr. Kimberly McFarland
Vein Doctor California
SUNY Downstate Medical Center
Our patients love us, you will too!
Your medical care has a 5-star track record. Our vein centers continuously receive 5-star ratings across all review sites, including google, facebook, and real self. Learn more about our patient success stories here.
My experience with this Vein Treatment Center has been more than pleasant and satisfactory. I was suffering from pain and swelling for a few years and the treatment provided worked 100%. I am so glad I took the decision to get my veins treated. The medical staff was super courteous and professional all the time.
I highly recommend the Vein Treatment Clinic. I finally decided in August this year to do something about my varicose veins. I had put it off for so many years and my veins were only getting worst. I was nervous about choosing the right medical group for treatment as you can hear horror stories. But from the moment I booked my first appointment over the phone I had a feeling I choose the right place. Dr Montoya is a fantastic vein specialist who is very professional, he also explains every detail of the procedure and puts you at ease. You can tell he takes great pride in his profession (I also have the legs to prove it now) But I can’t leave out Cassandra the Vascular Sonographer who just goes out of her way to make sure you are comfortable, answers any questions you have and is just a complete sweetheart who takes great pride in her job and is credit to the medical group.
Outstanding experience, highly recommend! Staff were professional and very helpful. The offices were clean and everyone adhered to COVID regulations. Dr. Montaya is an exceptional physician, patiently described all procedures, follow up treatment and calmly answered all my questions and helped me feel very safe and comfortable. And Cassandra a great tech! THANK YOU!
Did you know that most vein treatments are covered by insurances, including Medicare?
Questions? Call us (888) 827-7441
By emailing or contacting us, you are accepting the inherent privacy limitations of online communication. For more information, please read our Digital Communications document. Please respond “STOP” to any text messages to opt out.
FILL OUT THIS FORM FOR FREE INSURANCE VERIFICATION
Suffering from symptoms of vein disease?
These are the top Vein Treatments:
Sclerotherapy
RF Ablation
Venaseal
Clarivein
EVLT
Not sure what to choose?
Your vein treatment is customized based on your unique needs and preferences, and is performed utilizing the latest technology. Whether you are concerned about unsightly spider or varicose veins, or you are suffering from leg discomfort, heaviness, swelling, restlessness or muscle cramps, our vascular doctors have a vein treatment option for you. Learn more about our vein treatments here.
Not sure what is best for you? Book a consultation
If you have more questions regarding any of the treatments or conditions, please consult with one of our vein treatment doctors located in New York, New Jersey, Long Island, Maryland and California. All of our doctors are board certified and routinely perform all types of procedures with the highest standard of care and expertise.






