Men and women can suffer from chronic venous insufficiency (CVI), a condition in which veins in the legs (or hands) have faulty valves. These damaged valves fail to close properly, allowing deoxygenated blood to flow backward and pool in the veins. CVI can lead to varicose veins, spider veins, swelling, and even venous ulcers. If left untreated, it can result in serious complications. That’s why seeking an evaluation at a top vein treatment clinic is essential.
Symptoms of Chronic Venous Insufficiency
CVI can cause a range of symptoms, including:
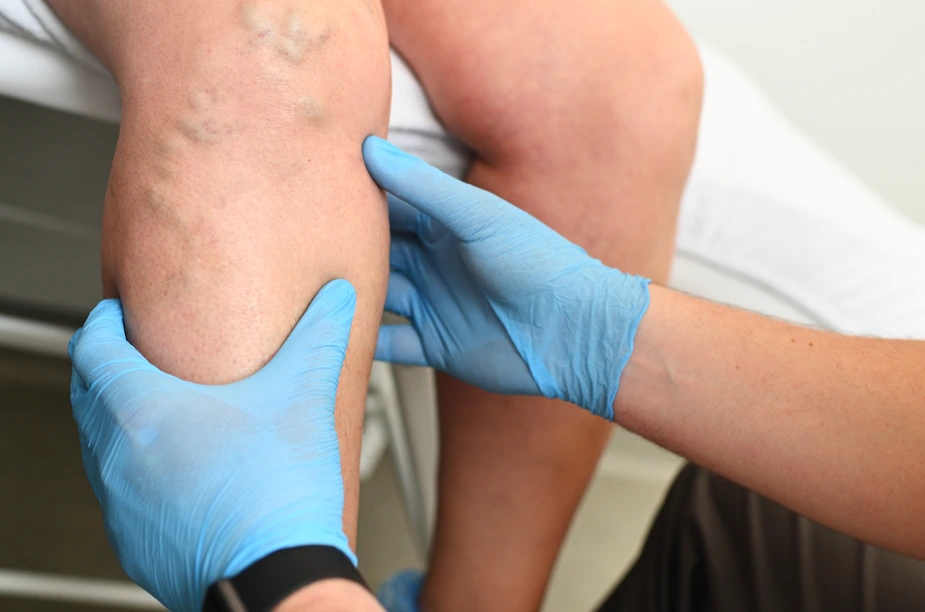
- Spider veins, reticular veins, and varicose veins
- Swelling around the ankles and legs
- Pain, cramping, or aching in the legs
- Itching, burning, or a feeling of heaviness
- Skin discoloration and venous ulcers

Risk Factors for CVI
CVI is influenced by several factors, including:
-
Genetics (family history of varicose veins or venous disease)
-
Obesity, which places excessive pressure on leg veins
-
Prolonged sitting or standing (work-related posture)
-
Pregnancy, which increases blood volume and hormonal changes
-
Deep vein thrombosis (DVT)
-
Leg injuries or muscle weakness
-
Phlebitis (swelling of superficial veins)
Top Treatments for Chronic Venous Insufficiency
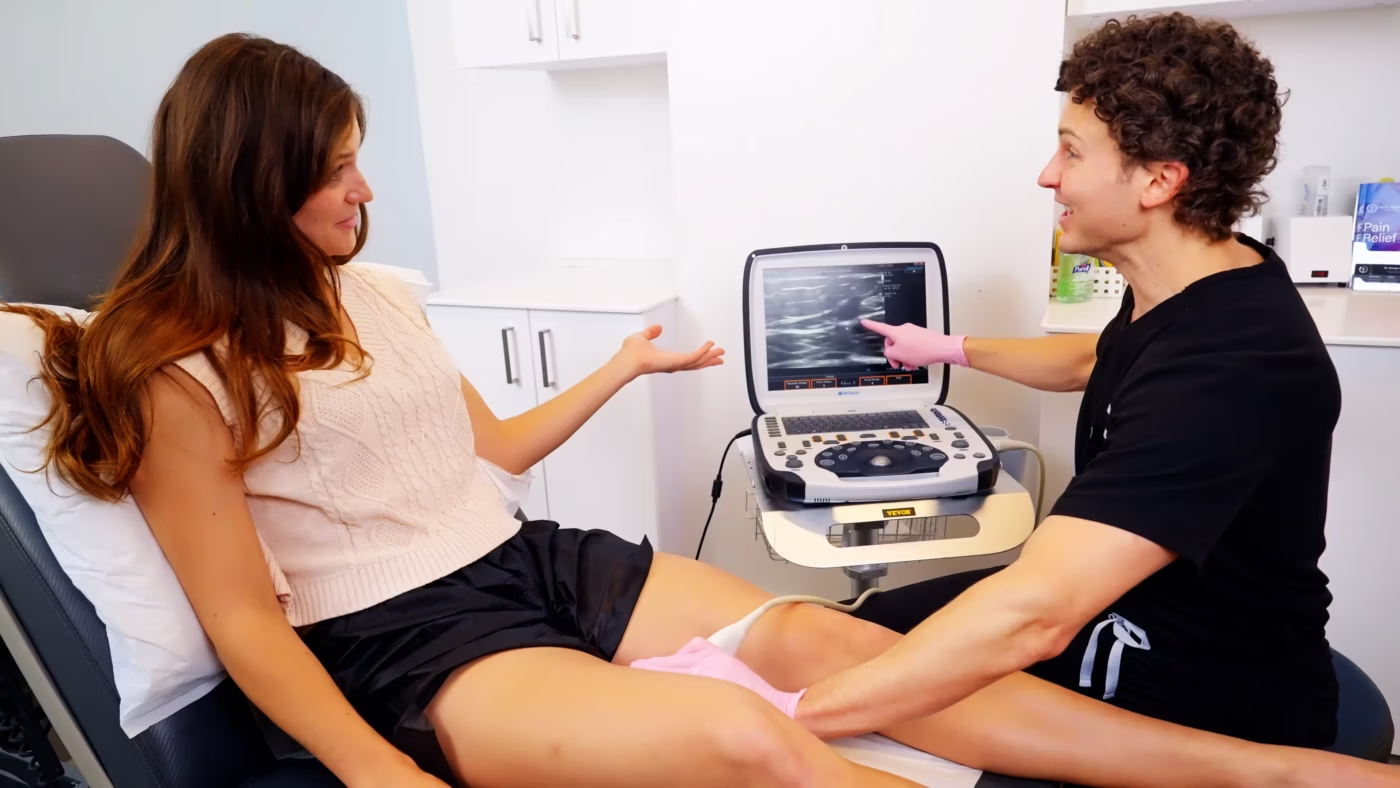
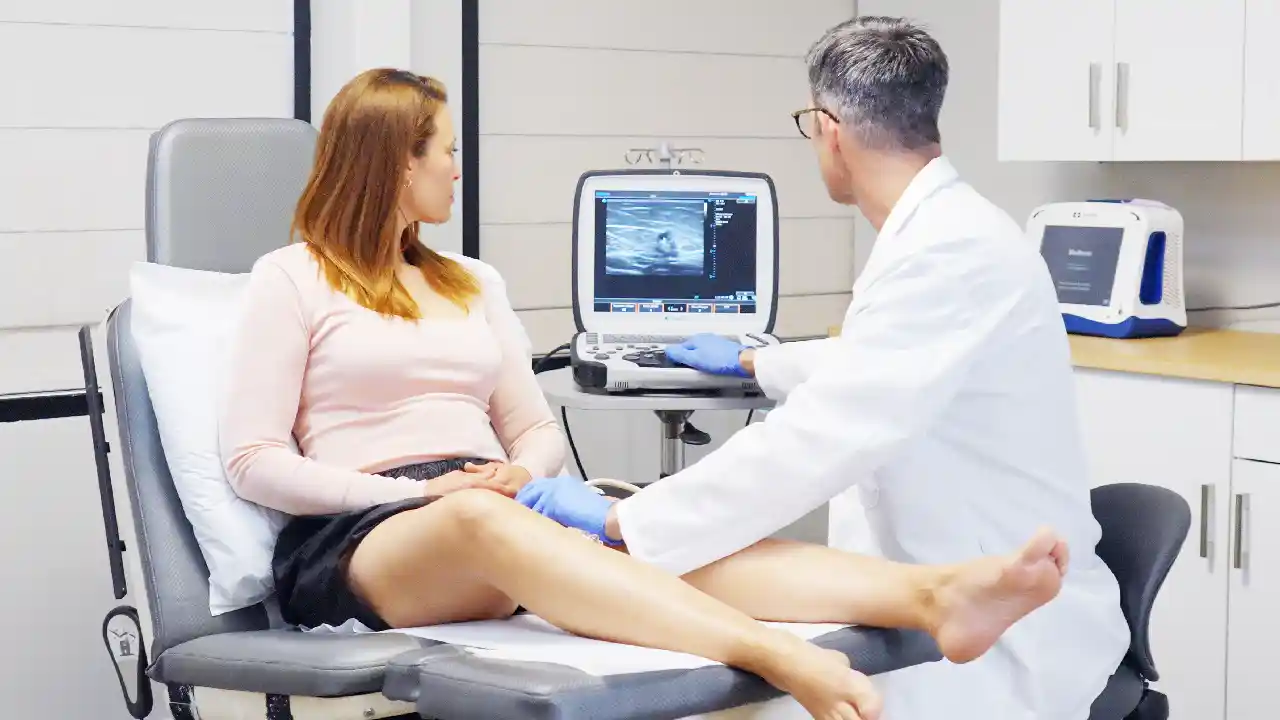
Vein Treatment Clinic offers minimally invasive treatments with quick recovery times. Every chronic venous insufficiency treatment with a comprehensive diagnostic evaluation using ultrasound technology to pinpoint the exact source of the problem.
Our expert vein doctors ensure you receive the most effective treatment for your specific condition.
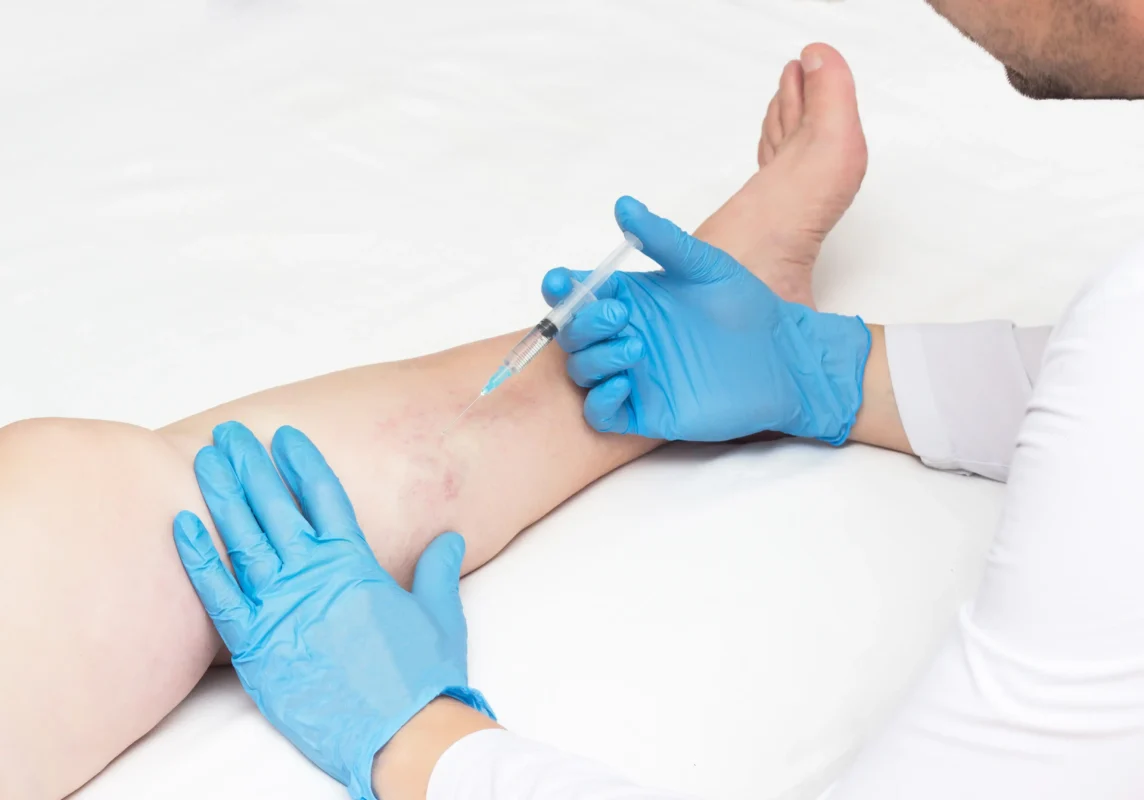
1. Sclerotherapy
- Best for: Spider veins and small varicose veins.
- How it works: A saline-based or foam solution is injected into affected veins, causing them to collapse and fade over time.
- Benefits:
- No anesthesia required
- Minimally invasive with minimal discomfort
- Fast recovery, with most patients resuming normal activities the same day
- Effective for cosmetic concerns and mild venous disease
2. Radiofrequency Ablation (RFA)
- Best for: Varicose veins and chronic venous insufficiency.
- How it works: A catheter delivers radiofrequency energy, which generates heat and collapses the vein.
- Benefits:
- Local anesthesia, with minimal discomfort
- High success rate (90%+ effective in closing diseased veins)
- Quick recovery, returning to normal activities within 24–48 hours
- Lower risk of complications compared to surgical vein stripping
3. Laser Ablation (EVLA)
- Best for: Treating larger varicose veins with minimal invasiveness.
- How it works: A fiber-optic laser is inserted into the affected vein, delivering precise heat that shrinks and seals the vein.
- Benefits:
- Highly precise, ensuring effective treatment of targeted veins
- Minimally invasive, performed under local anesthesia
- Short recovery time, with most patients walking immediately after
- Clinically proven with long-term success
4. ClariVein
- Best for: Patients looking for an alternative to heat-based treatments.
- How it works: A mechanochemical catheter delivers a sclerosing agent while rotating to close the vein.
- Benefits:
- No heat or risk of nerve damage
- Requires fewer injections than traditional sclerotherapy
- Quick and virtually painless procedure
- Minimally invasive with same-day recovery
5. Varithena
- Best for: Medium to large varicose veins that require a foam-based approach.
- How it works: A specialized foam sclerosant is injected to collapse and shrink the affected veins.
- Benefits:
- Effective for larger varicose veins that don’t respond to standard sclerotherapy
- Quick procedure, taking less than 30 minutes
- No downtime required, allowing immediate return to daily activities
- Minimal discomfort, with mild swelling as the most common side effect
Schedule Your Consultation
If you experience symptoms of chronic venous insufficiency, varicose veins, or spider veins, don’t wait to seek treatment. Early intervention prevents complications like leg ulcers, severe swelling, or chronic pain. Our expert team at Vein Treatment Clinic can guide you through the best treatment options and help verify your medical insurance coverage to minimize out-of-pocket costs. Many insurance plans cover vein treatments when deemed medically necessary, and we’ll assist you in navigating the approval process.