You’re getting ready for a day at the beach, only to be reminded by the bulging, unsightly varicose veins snaking down your legs. You quickly decide to wear longer clothing, hiding your discomfort and hoping no one notices. It’s not just about aesthetics; those veins might be causing you pain, swelling, and a heavy sensation that lingers long after the day is over.
If this sounds familiar, you’re not alone. Varicose veins are a common issue affecting millions of people. Fortunately, medical advancements have led to minimally invasive treatments that can alleviate the symptoms and restore the appearance of your legs. At Vein Treatment Clinic, we offer a range of cutting-edge varicose vein treatments that fit your lifestyle. This article will introduce you to the top five treatments available today and explain why choosing Vein Treatment Clinic for your care can make all the difference.
Sclerotherapy
Sclerotherapy is often regarded as the gold standard for treating small varicose veins and spider veins. It involves injecting a sclerosant directly into the affected veins. The solution irritates the vein walls, causing them to collapse and eventually be reabsorbed by the body. Over time, the treated veins fade from view. Sclerotherapy usually takes about 30 minutes. You’ll be able to walk immediately afterward and can return to your normal activities the same day.
Insurance Considerations
While sclerotherapy is often considered a cosmetic procedure, it can be covered by insurance if it’s part of a treatment plan for chronic venous insufficiency. If you’ve been diagnosed with this condition, your insurance may cover your entire treatment. Contact us to request insurance verification and find out if your sclerotherapy is covered.
Radiofrequency Ablation
Radiofrequency ablation (RFA) is another highly effective, minimally invasive treatment for varicose veins and underlying chronic venous insufficiency. This procedure uses radiofrequency energy to heat the inside of the vein, causing it to collapse and seal shut. Over time, the body reroutes blood flow to healthier veins, and the treated vein is absorbed and disappears. The procedure is typically performed under local anesthesia and takes less than an hour. Most patients experience little to no pain during and after the procedure.
VenaSeal
Unlike other treatments that use heat or chemicals, VenaSeal involves using medical adhesive to close the vein. During the procedure, a small amount of adhesive is delivered to the affected vein through a catheter. The adhesive seals the vein shut, and the body naturally reroutes blood flow to nearby healthy veins. VenaSeal doesn’t require tumescent anesthesia, which is often necessary for other treatments. This reduces discomfort during the procedure and eliminates the need for multiple needle sticks.
Clarivein
Clarivein combines mechanical and chemical methods to treat varicose veins. During the procedure, a rotating catheter is used to damage the vein’s lining while delivering a sclerosant solution to seal the vein shut. This dual-action approach makes Clarivein highly effective, especially for veins that might not respond to other treatments. Clarivein doesn’t require heat or tumescent anesthesia, making it a less painful option with quicker recovery. The procedure typically takes 30 minutes, and most patients return to their daily activities immediately.
Ambulatory Phlebectomy
Ambulatory phlebectomy is a minimally invasive surgical procedure used to remove surface varicose veins. During this procedure, small incisions are made along the length of the vein, and the vein is removed using a specialized hook. The incisions are so tiny that they don’t require stitches, and any scarring is minimal. This treatment is particularly effective for larger varicose veins that bulge above the surface of the skin. It can be performed in conjunction with other treatments, such as RFA, to achieve the best possible results.
Advantages of Seeking Varicose Vein Treatment at VTC
Expertise of Board-Certified Vein Doctors
At Vein Treatment Clinic, you’ll be in the hands of board-certified vein doctors. Our physicians are certified by the American Board of Venous and Lymphatic Medicine and have completed rigorous training in varicose vein treatments. This ensures that you receive the highest standard of care from professionals who are committed to achieving the best outcomes for their patients.
State-of-the-Art Technology
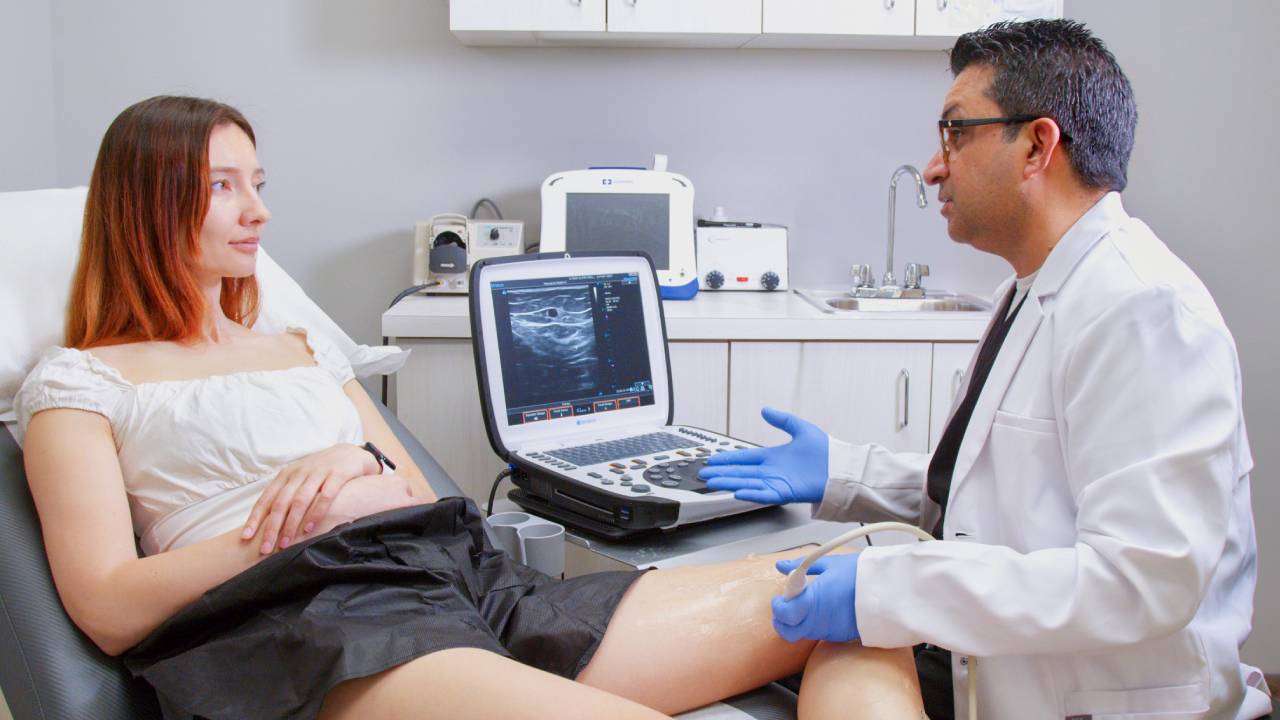
Our vein clinics are equipped with the latest technology to diagnose and treat varicose veins. We use advanced imaging techniques, such as duplex ultrasound, to identify the root cause of varicose veins before recommending a treatment plan. This allows us to tailor our approach to your specific needs, ensuring that you receive the most effective treatment possible.
Personalized Care and Treatment Plans
We understand that every patient is unique, which is why we offer personalized care and treatment plans. After a thorough evaluation, our vein specialists will create a customized plan that addresses your specific condition and goals. Whether you need sclerotherapy, RFA, or any other treatment, we ensure you feel confident every step of the way.
Insurance Coverage Verification
At Vein Treatment Clinic, we offer insurance verification to all our patients. Most of our varicose vein treatments are covered by medical insurance when they are deemed medically necessary. We’ll work with your insurance provider to ensure that you receive the coverage you’re entitled to, making your treatment as affordable as possible.
Dealing with varicose veins can be more than just an aesthetic issue—it can affect your quality of life. Fortunately, minimally invasive vein treatments like those offered at Vein Treatment Clinic can help you reclaim your confidence. With state-of-the-art vein clinics in New York, Long Island, California, Maryland, and New Jersey, getting the care you need has never been more convenient—contact us to schedule your consultation today.