Table of contents
Get treated by vein treatment industry leaders
Are Spider Veins Covered by Insurance?
Medically verified
Last updated on 1/29/2026

By Dr. Michael Nguyen
Vein Doctor at Vein Treatment Clinic
Harvard Medical School
Board Certified by the American Board of Venous and Lymphatic Medicine
Many patients ask whether spider vein treatment is covered by insurance, especially when visible veins are accompanied by discomfort or recurring symptoms.
In most cases, spider veins are considered cosmetic. However, insurance coverage depends on whether treatment is deemed medically necessary.

Understanding how insurance companies evaluate spider vein treatment helps patients plan care and avoid unexpected costs.
If you’re unsure whether your spider veins may qualify for insurance coverage, a vein evaluation can help clarify your options.
Are spider veins usually considered cosmetic?
Yes. Most spider veins are classified as cosmetic by insurance providers because they do not typically cause significant medical problems.
When treatment is performed solely to improve appearance, insurance generally does not cover the cost.
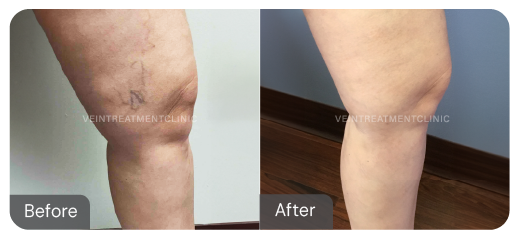
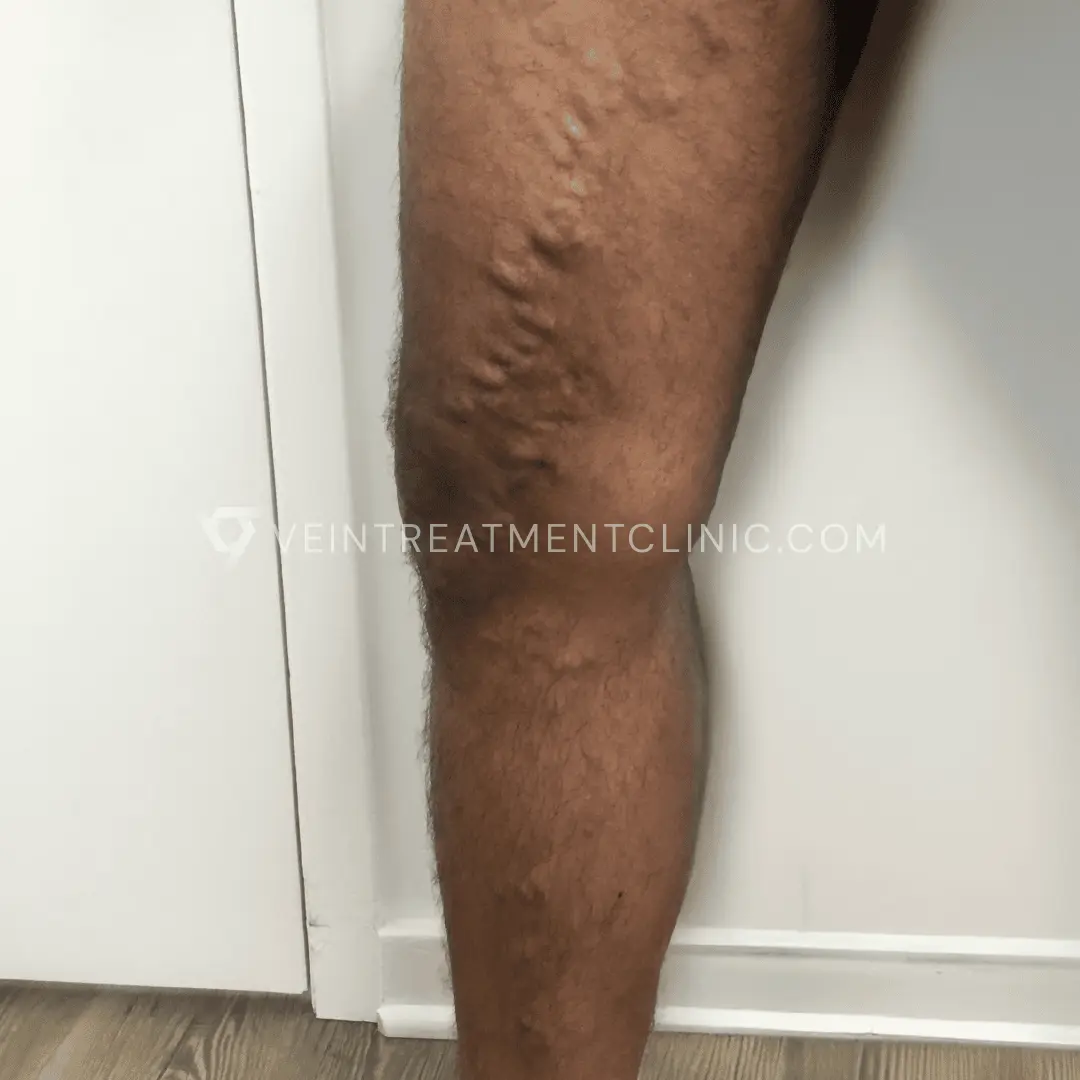
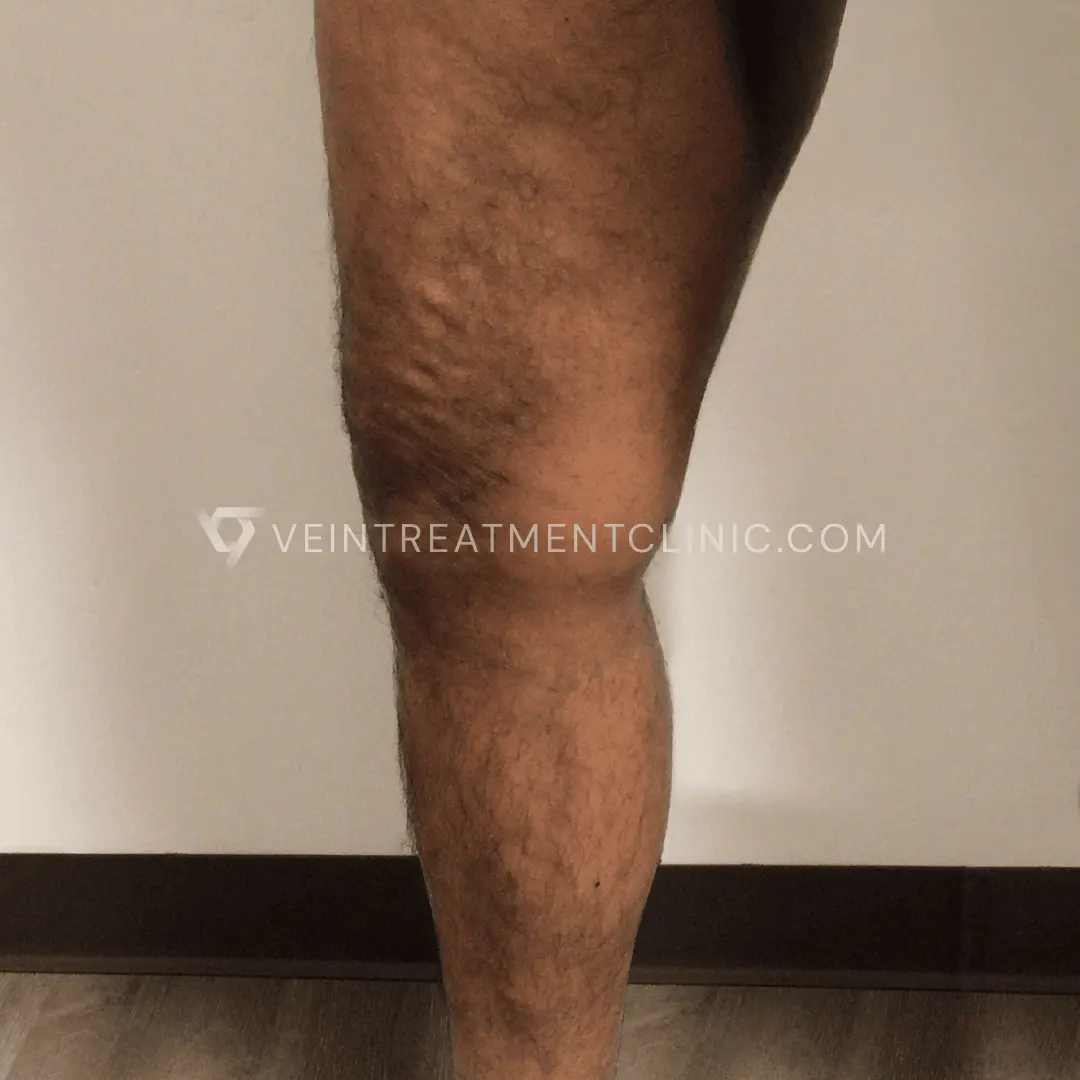
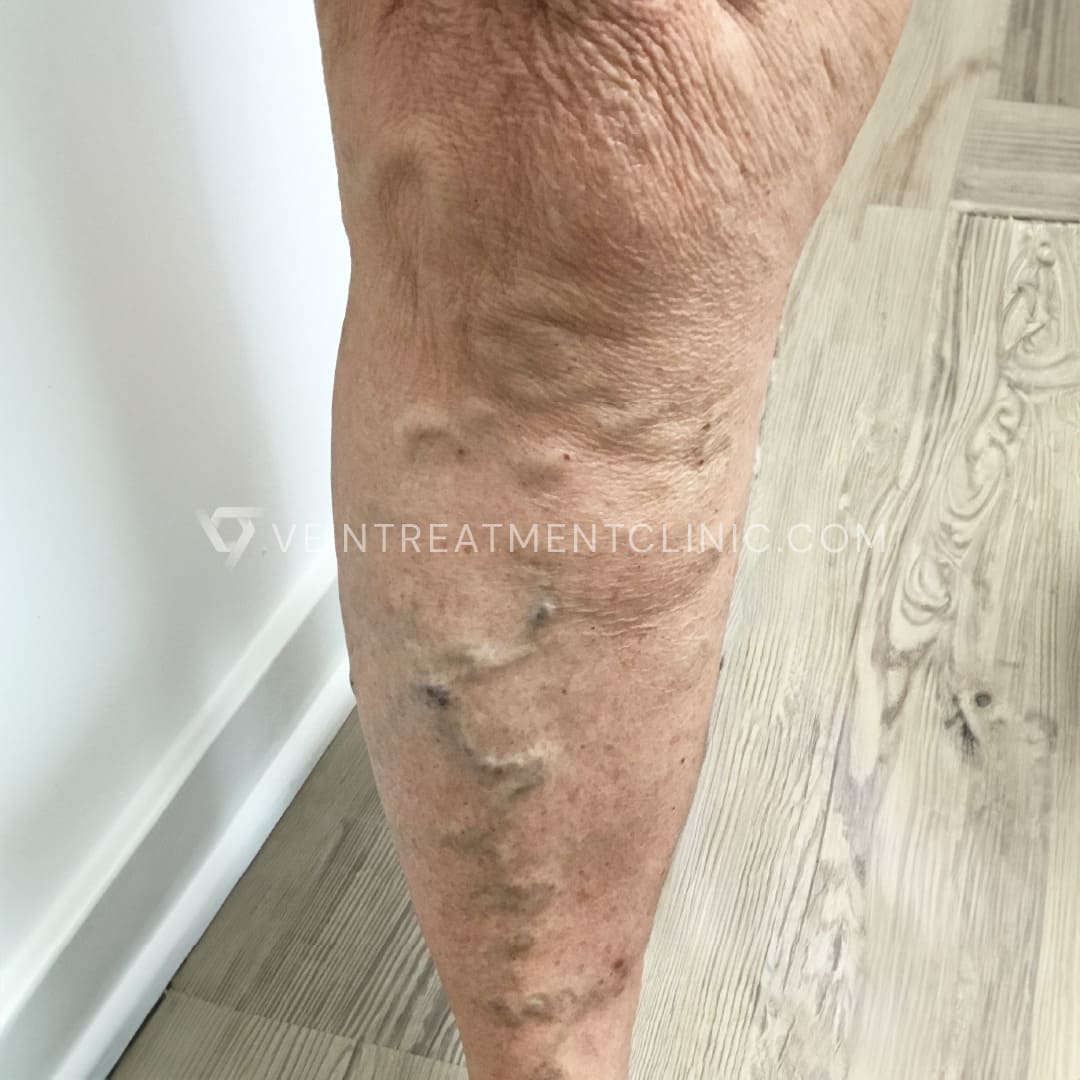
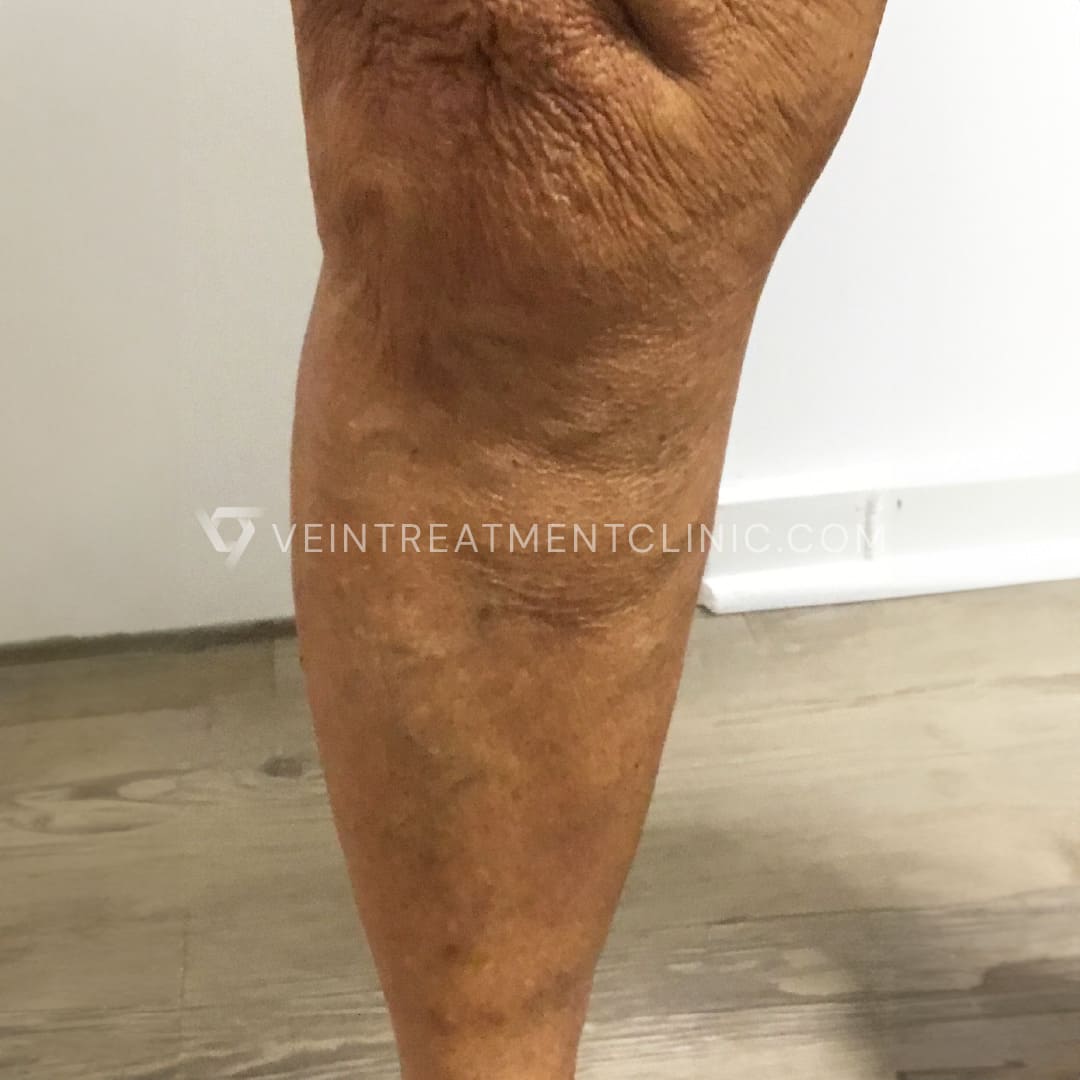
Spider Vein before and after treatment pictures.
Results may vary according to each case.

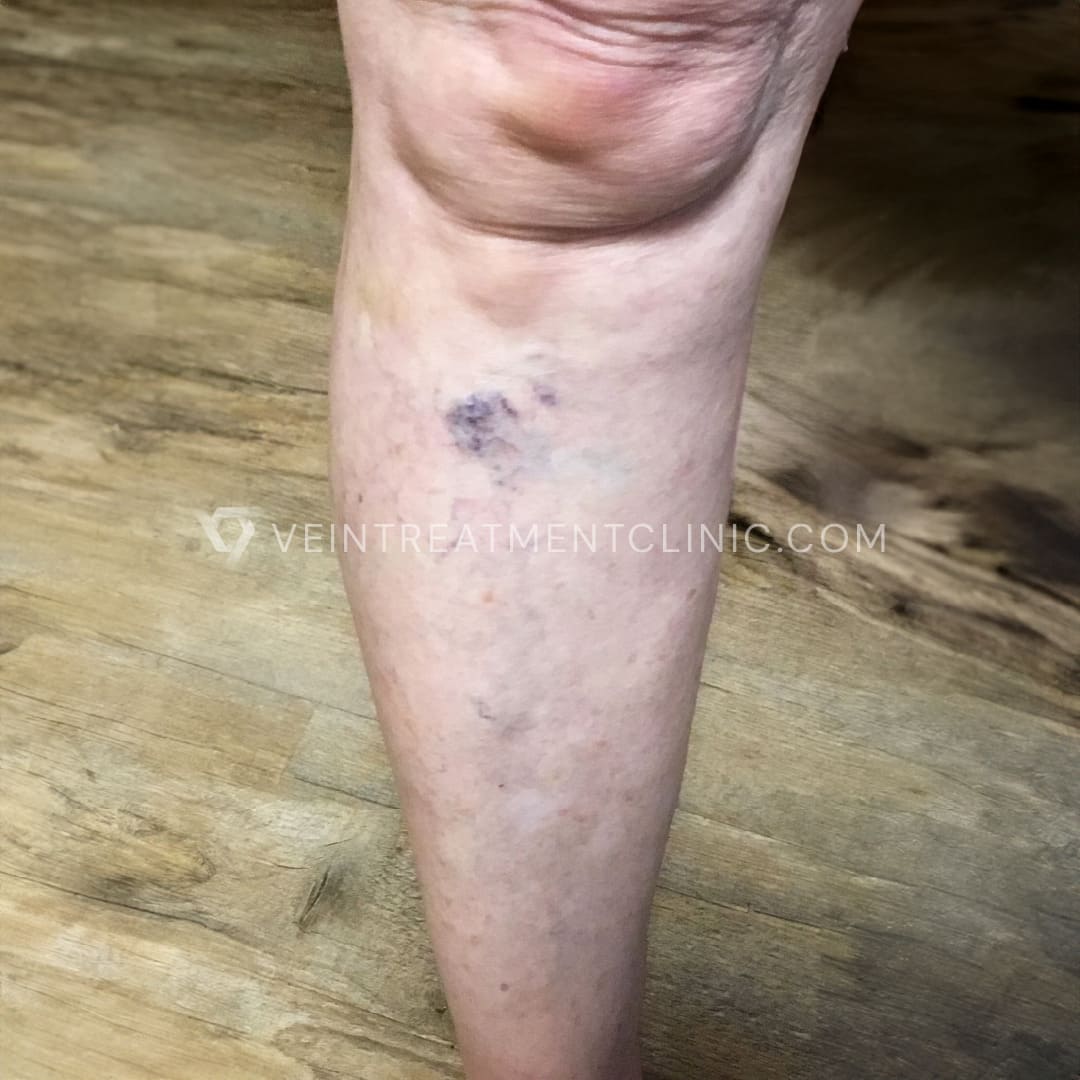
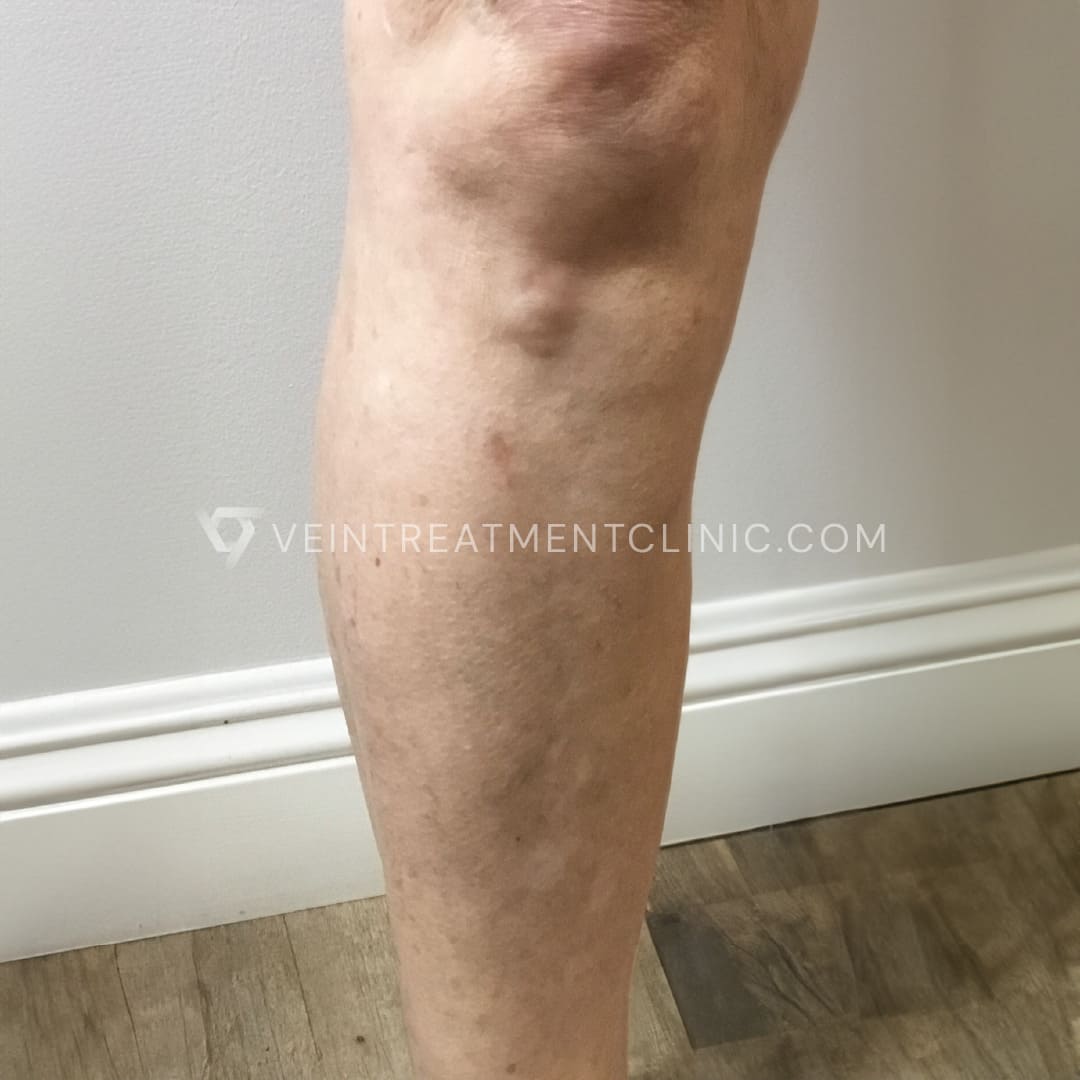
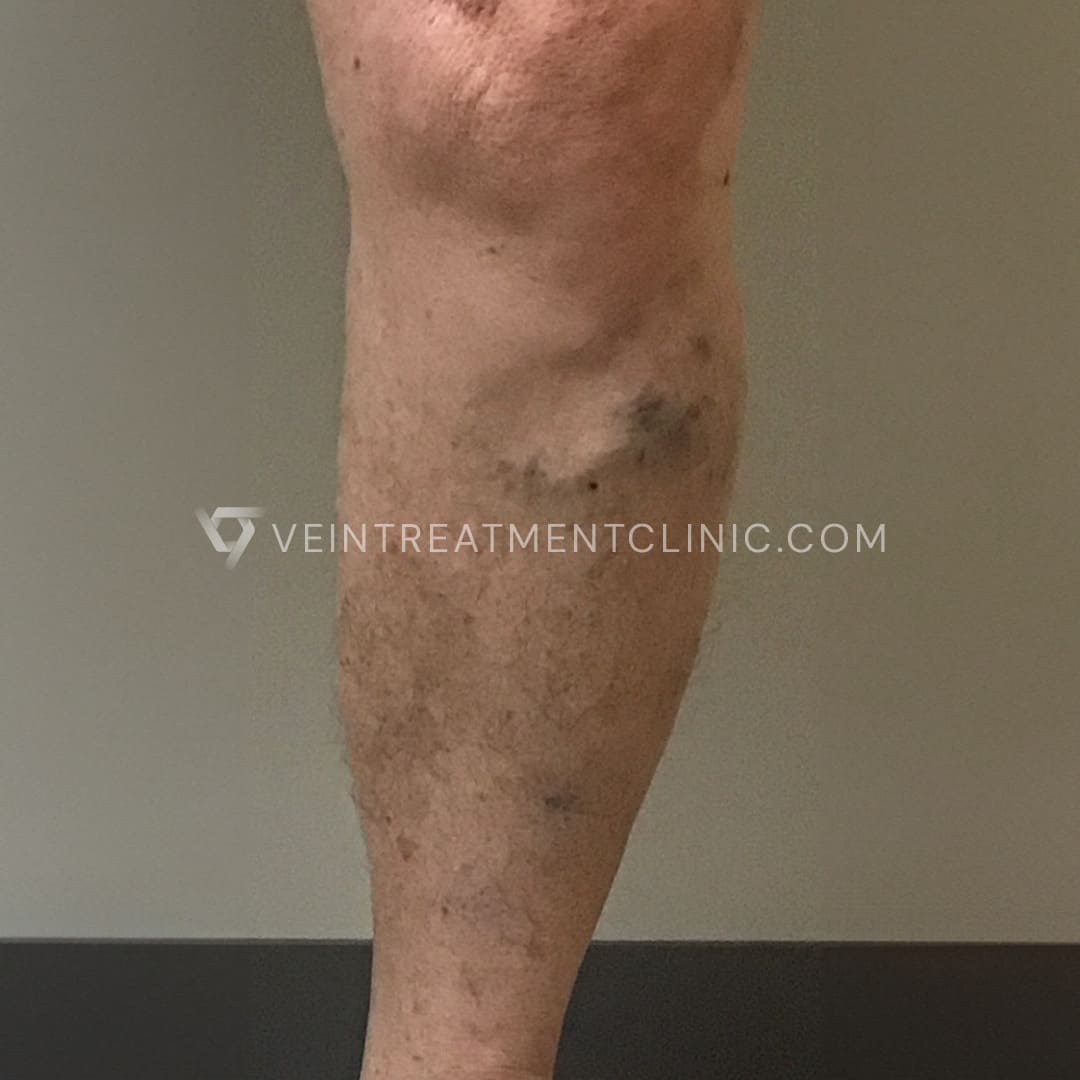
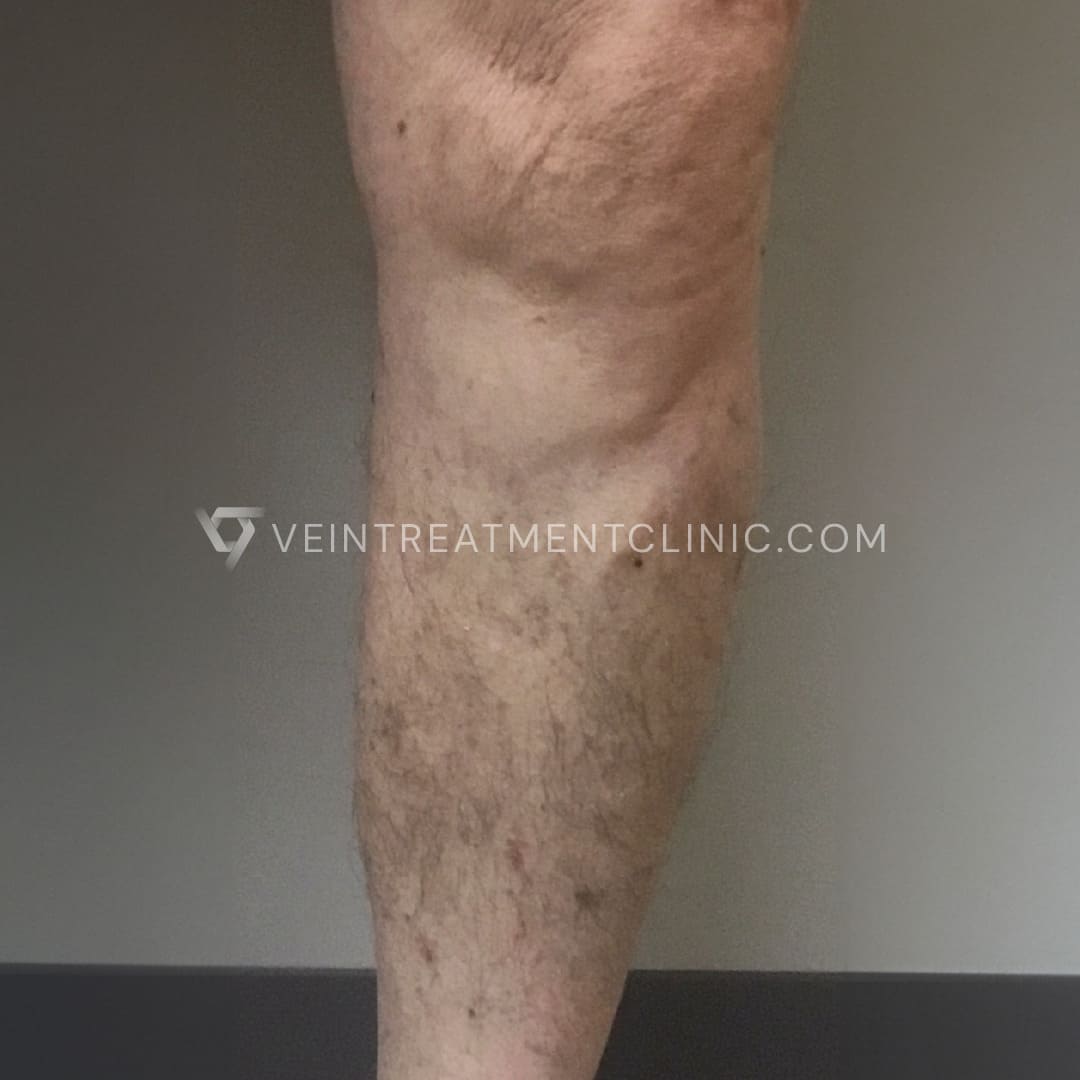
Spider Vein before and after treatment pictures.
Results may vary according to each case.
When might spider vein treatment be considered medical?
Spider vein treatment may be considered medical when veins are associated with symptoms such as pain, burning, itching, swelling, or recurrent inflammation.
In these cases, insurance may evaluate whether spider veins are linked to underlying venous insufficiency.
Does insurance cover sclerotherapy for spider veins?
Sclerotherapy for spider veins is usually not covered when performed for cosmetic reasons.
If sclerotherapy is used as part of treatment for medically significant vein disease, coverage may apply depending on the diagnosis and documentation.
Symptom Checker
What role does vein ultrasound play in insurance decisions?
Insurance companies often require ultrasound evidence of venous reflux or valve failure to consider treatment medically necessary.
Ultrasound helps determine whether spider veins are isolated or related to deeper vein disease.
Get a Peek Inside Your Veins—Book Your Ultrasound Evaluation.
How do insurance companies define medical necessity?
Medical necessity is typically based on documented symptoms, physical exam findings, and imaging results.
Common criteria include pain, swelling, skin changes, bleeding, or ulceration related to vein disease.
What costs are patients responsible for if treatment is cosmetic?
When spider vein treatment is cosmetic, patients usually pay out of pocket.
Costs vary based on the number of veins treated, the number of sessions needed, and the treatment method used.
Do insurance plans differ in coverage?
Yes. Coverage criteria vary widely between insurance plans and carriers.
Some plans require prior authorization, documentation of conservative treatment, or specific diagnostic findings.
How can patients find out what their insurance covers?
The best way to determine coverage is through a vein evaluation followed by a benefits review.
Many clinics can help verify insurance coverage and explain expected costs before treatment begins.